The right care at the right time
Utilization management and the Devoted mission
At Devoted Health, we strive to offer every member the kind of healthcare experience that we would want for our own family members.
For our Utilization Management team, that means ensuring our members can access clinically appropriate, best-in-class care — provided at the right time and in the right place.
We aim to make this process as smooth as possible for both our members and providers, while being thoughtful stewards of Medicare resources.

“I was with Devoted when I had my surgery this summer. It was just carefree. I didn't have to jump through hoops like I did with my old insurance company. [Devoted] just approved the surgery immediately… bing bang boom, it was taken care of. There was no stress.”
— Judy C., Devoted Health member
How we support our members
We’re committed to driving excellent health outcomes for all our members, so we:
- Design plans with benefits that meet members’ health needs and help them thrive
- Staff our chat and phone lines with friendly, knowledgeable Member Service Guides to help members make the most of their benefits
- Regularly review our performance to ensure that our Utilization Management team is providing excellent service to all members
Getting members the right care
Our Utilization Management team works to make sure our members get care that’s safe, effective, and in line with Medicare guidelines. Every request we review is guided by 2 goals:
- Helping our members get the care that’s most appropriate for their health needs
- Avoiding care that could be unnecessary, ineffective, or even harmful
Overall, we approve 94.6% of medical prior authorization requests* from our members and providers (based on 2025 data). And when we deny a request, we’re here to support members in getting the care they need. For example, if we deny out-of-network care for an HMO plan member, we can help them find nearby in-network providers who can provide the requested care.
In 2025, 88.5% of medical requests were submitted as standard and 11.5% were submitted as expedited.
- Standard medical requests: 95.1% approved, 4.9% denied
- Expedited medical requests: 90.7% approved, 9.3% denied
The chart below shows the distribution of all medical authorization requests we received in 2025, by outcome (approved or denied) and type of request (standard or expedited).
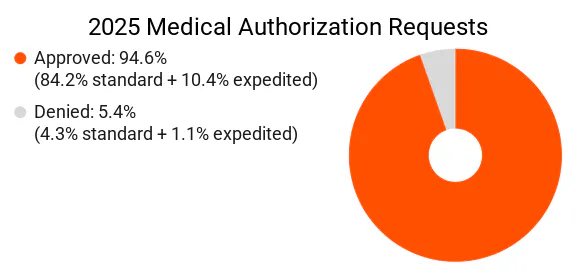
Getting members care at the right time
We return decisions fast — much faster than what Medicare requires — so members don’t face delays getting needed care. In 2025, we returned more than half of all decisions in less than 2.5 hours, and our timeframes averaged as follows:
- Standard requests: Less than 1.5 days — compared to the 14-day Medicare timeframe for 2025**
- Expedited requests: Less than 10 hours — compared to the 72-hour Medicare timeframe for 2025
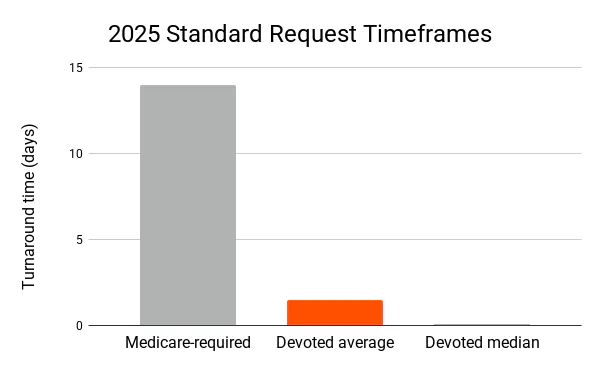
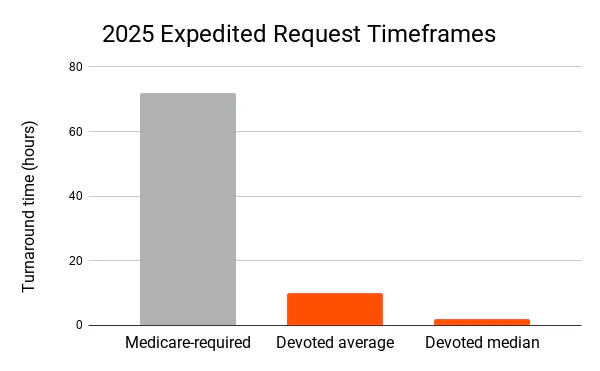
Extended review
In very rare cases, we may need to take longer than the Medicare timeframe to gather evidence, evaluate the request, and arrive at a decision. In 2025, this happened only twice out of more than 170,000 total requests.
Appeals
When a member or provider disagrees with a decision we’ve made, they have the right to appeal. For each appeal, we carefully re-consider our decision, taking into account any new information that a member or provider may have shared with us. We apply the same standard as in our initial reviews:
- Helping our members get the care that’s most appropriate for their health needs
- Avoiding care that could be unnecessary, ineffective, or even harmful
We strive to make the right decision the first time and explain our rationale clearly, so that appeals are rare. In 2025, less than 10% of standard denials were appealed — that’s less than 1% of all standard requests.
*In 2025, more than 6% of standard requests were pre-service coverage determinations for supplemental dental services, which differ significantly from medical coverage determinations. Dentists often submit these requests as a way to check what the plan covers — resulting in “denials” where the plan doesn’t cover a specific procedure, or where the requested services are approved, but the cost of those services exceeds the member’s remaining allowance amount.
The approvals data above do not include supplemental dental coverage determinations. With these coverage determinations included:
- Standard requests: 91.8% approved, 8.2% denied
- Expedited requests: 90.7% approved, 9.3% denied
**Note: Starting January 1, 2026, the Medicare timeframe for standard prior authorizations is 7 days.